GET INFORMED

UNDERSTANDING BRAIN INJURY
Years ago, brain injury was known as Traumatic Brain Injury (TBI) and was the result of a blow or jolt to the head such as from a fall or hitting one’s head in a car crash. The term used now is acquired brain injury caused from tumour, aneurysm, stroke, a blow or jolt to the head, concussions, near-drowning, and falls. A blow to the head can result from a bike or a motor vehicle crash, a sporting or small wheeled vehicle incident, abuse or a fall.
You do not have to lose consciousness to sustain a brain injury. The effects of a brain injury are often lifelong and debilitating. A brain injury can result in cognitive and behavioural problems and include personality changes, memory loss, and the inability to return to work.

TOP CONCERNS
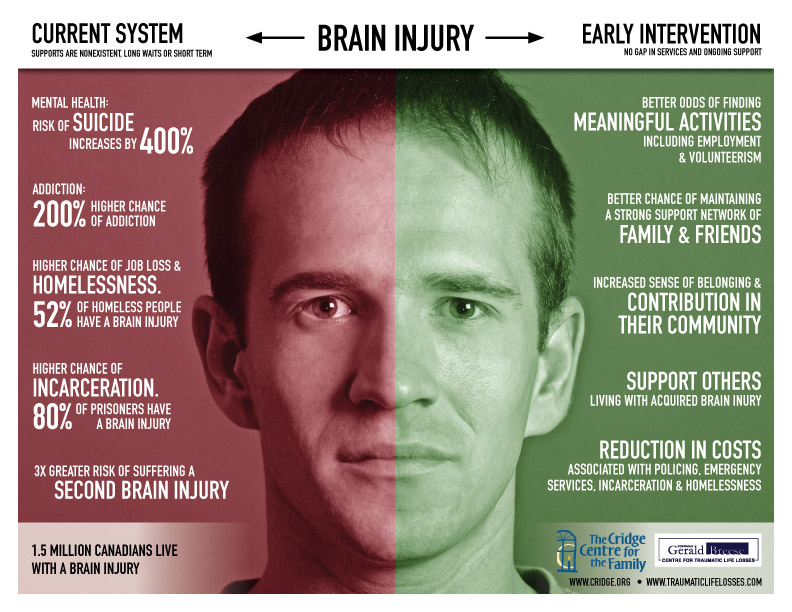
- 1.5 million Canadians live with a brain injury – these are only the documented cases. The numbers are greater when considering domestic violence, dangerous substance use, and those who have gone undiagnosed although they sought medical help.
- The current economic burden of acquired brain injury, combined with treatment, is an estimated $12.7 billion per year (Northern Brain Injury Association).
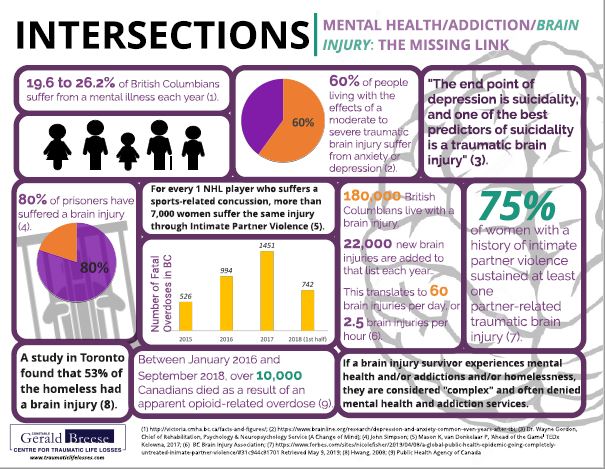
- Over 80% of those incarcerated have a brain injury and 60% of this group suffered their first brain injury as a child and often at the hand of abuse (John Simpson).
- 52% of the homeless have sustained a brain injury and over 70% of this population became homeless after their first brain injury.
- Brain Injury Survivors are at risk for significant mental health and addiction challenges, yet they are often denied service.
- The incidence and prevalence of brain injury surpasses HIV/Aids, Spinal Cord Injury, Breast Cancer and Multiple Sclerosis combined.
WAYS TO HELP
- Keep informed on what is happening with research and what is happening in your area. Visit brainstreams.ca to keep up-to-date on trends, information, and to learn about others on this journey
- Connect with the local Brain Injury Association in your town, city or province to access programs and supports
- Contact your local health authority to determine what services are available to you and your family
- Write to your MLA and MP and share your story and any challenges you have accessing services for brain injury, mental health or addiction and ask them to support an integrated health strategy to ensure that brain injury services and supports are adequately funded across the country.
“Brain injury remains the orphan in our healthcare system. No one wants it yet everyone assumes someone else is taking care of it.”
~Janelle Breese Biagioni
UNDERSTANDING MENTAL HEALTH
Looking after our mental health, adults and children alike, is an important part of life. Our mental health includes our psychological and social well-being and it has an impact on how we think, feel, and act in our daily life. The state of our mental health determines how well we handle stress, make choices in our daily lives and how we relate to others. Taking care of our mental health needs to become a part of everyday conversations, workplace strategies, and school environments.
Our mental health is impacted by events that happen to us. For example, it is a normal response to feel sad or depressed after the death of a loved one. It is not uncommon to feel anger when a situation is unfair or unwarranted or when we have been taken advantage of. It is important to work through these thoughts, feelings, and emotions.
A person’s mental health is also impacted by mental health disorders/illnesses such as Anxiety & Panic Disorder, OCD or PTSD. If you or a loved one are experiencing symptoms or have areas of concerns about your mental health and wellbeing, please immediately contact your healthcare practitioner, local emergency room, or call the crisis line.

1-800-SUICIDE (1-800-784-2433) – call if you are having thoughts of suicide. Support is available 24/7.
310-MENTAL HEALTH (310-6789)- You do not need to add 604, 778, 0r 250 when dialing this numbers. Call for 24/7 emotional support and to learn of resources specific to mental health in British Columbia.
TOP CONCERNS
- Between 19.6% & 26.2% of British Columbians will experience a mental illness each year (CMHA)
- Approximately 84,000 children/youth in BC have been diagnosed with a mental disorder but less than 1/3 are receiving treatment
If you experience any of the following, please seek medical advice:
- Has your eating and sleeping patterns changed?
- Are you have difficulty participating in daily activities?
- Are you experiencing fatigue or low energy or unexplained aches and pains?
- Do you feel hopeless or helpless?
- Has your drinking, smoking, eating or use of drugs increased?
- Do you have persistent thoughts or hear voices?
- Are you harming yourself or thinking of harming yourself or others?
*Note: This is not an exhaustive list of symptoms or concerns – if you have any concerns, questions or symptoms, seek medical advice.
WAYS TO HELP
You can help yourself or a loved one by:
- Seeking the help of a professional as needed
- Help your loved one get connected with others or if this is for you, seek out groups where you can receive support
- Feed your mind and soul with positive information – read positive material, listen to positive meditations and/or music.
- Engage in physical activity – it needn’t be strenuous – go for a walk, bike ride or a swim.
- Ensure you have structure – go to bed at a certain time and get up at a certain time – eat at regular intervals even if it is something small.
- Go out and do something for someone else who could use the support – helping others actually gives our outlook on life a major boost!
- Look up “coping skills” on the Internet, YouTube or in the library – there is lots of information to help you implement new strategies.
- Pace yourself!
UNDERSTANDING ADDICTION
Addictions is a very complex topic! People everyday are struggling with addictions that include such things as: drugs, alcohol, gambling, sex, food and work. When these elements hijack life and become all-consuming for the person, it often becomes a problem in their ability to fulfill daily commitments, maintain employment and/or relationships, and to stay safe. Addictions, much like brain injury and mental health challenges, impact the entire family.
An important understanding is to know that the person who lives with an addiction is not being lazy, lacks will power or is unmoral. More often than not the person is attempting to deal with pain – physical pain, emotional pain, spiritual pain. We believe addictions are trauma based and prefer to ask, “what has happened to you” rather than “what is wrong with you”.

Note: If you need help or are with someone who has overdosed, IMMEDIATELY call 9-1-1 and follow the Save Me protocol while waiting for first responders.
SAVE ME PROTOCOL retrieved from the British Columbia Government website:
Know that you are protected by the new Canadian Good Samaritan law. You will not be arrested or charged for drug possession by police if you call 9-1-1 to save the life of someone who overdoses.
SAVE ME
Stimulate. Check if the person is responsive, can you wake them up?
Airway. Make sure there is nothing in the mouth blocking the airway, or stopping them from breathing.
Ventilate. Help them breathe. Plug the nose, tilt the head back and give one breath every 5 seconds.
Evaluate. Do you see any improvement?
Muscular injection. Inject one dose (1cc) of naloxone into a muscle. Click here to learn more about Naloxone and how to safely administer it.
Evaluate and support. Is the person breathing? If they are not awake in 5 minutes, give one more 1cc dose of naloxone.
If you need to leave the person alone for any reason, place them into the recovery position before you leave to keep the airway clear and prevent choking.
- Turn onto the side.
- Place hand under head to support the head.
- Place the top leg slightly in front of the leg touching the ground and place the knee to the ground to prevent the body from rolling into the stomach.
TOP CONCERNS
- 1 in 5 Canadians / nearly 1,000,000 in BC suffer from an addiction
- The Opioid Crisis is escalating with nearly 4,000 Canadians dying from an overdose in 2017
- In BC, death from overdoses continue to increase. 523 people died n 2015, 974 in 2016 and 1,399 in 2017
- 90% of overdoses are unintentional
- Many of the fatalities occur at home
- The Canadian Institute for Health reports that above the fatalities, there are 17 people across Canada taken to the hospital daily for opioid poisoning.
WAYS TO HELP
- If you or a loved one are struggling with an addiction and need help call 1-800-663-1441 to obtain information about Alcohol and Drug Programs or for a referral.
- Educate yourself in supporting a loved one with an addiction – this also means taking care of yourself.
UNDERSTANDING TRAUMA
Trauma is the result of living through a distressing event in life. The long-lasting effects of trauma may leave a person feeling powerless, hopeless, helpless, or filled with shame and/or fear. The stress of the experience can manifest in the person experiencing an impact to their own sense of personal safety, their sense of self or who they are. In turn, trauma may impact their ability to regulate emotions, maintain relationships, and manage day-to-day.
The long-lasting effects of trauma may leave the person feelings of powerlessness, shame, hopelessness, helpless, and filled with fear. It interferes with how they manage daily living.

Traumatic experiences may occur when we are children from neglect or abuse or from witnessing chaos and violence in the home. It may occur as an adult if a person has been in a motor vehicle crash, assaulted, lived through a natural disaster, been in a violent situation and/or suffered the unexpected and sudden death of a loved one.
HOW TO IDENTIFY THE SIGNS
- A person may experience a vast list of “normal” responses after trauma. This can include confusion, panic, a sense of chaos, anger, sadness, outbursts, hopelessness, anxiety, withdrawal.
- When the responses above do not dissipate or soften with time, it is important the person seek advice with a healthcare practitioner who has been trained in trauma care.
- Interview potential counsellors and ensure you have a connection with him or her – it takes courage to share your story and walk the path of healing so you have the right to do it with someone who is the right fit.
HOW IT AFFECTS EVERYDAY LIFE
- Don’t allow yourself to isolate – reach out to others who can be a support to you and who have been trained to help with trauma.
- Maintain structure – eating, sleeping and light exercise
- Look into effective mindfulness techniques, meditation, and Cognitive Behavioural or SomaticTherapy.
- Maintain social connections -even if it is with a few select friends. Allow yourself to experience “joy” and fun in life.
- Help someone else – so many people could use a “loving listener” or benefit from a little kindness in their day and you will feel a little better yourself.
